STONY BROOK, NY, October 19, 2015 – Electrical waves regulate the rhythm of the heartbeat, and when those signals go awry, the result is a potentially fatal arrhythmia. Now, a team of researchers from Stony Brook University and Oxford University has found a way to precisely control these waves – using light. Their findings are published in the Advance Online edition of Nature Photonics.
There are currently two options for cardiac patients to keep these electrical waves in check: electrical devices (pacemakers or defibrillators) or drugs (eg beta blockers). However, these methods are relatively crude: they can stop or start waves but cannot provide fine control over the wave speed and direction. This is like being able to start or stop a boat but without the ability to steer it. So, the researchers set out to find ways to steer the waves, borrowing tools from the developing field of optogenetics, which to date has been used mainly in neuroscience.
Optogenetics uses genetic modification to alter cells so that they can be activated by light. The technology has mainly been used to activate individual cells or to trigger electrical signals that travel from cell to cell as “excitation waves” in tissue. According to Co-author Emilia Entcheva, PhD, Professor of Biomedical Engineering, Physiology & Biophysics, and Cardiology at Stony Brook Medicine, in the paper “Optical control of excitation waves in cardiac tissue,” the team details how they used optogenetics to precisely control the activity of millions of cardiac cells.
“When there is scar tissue in the heart or fibrosis, this can cause part of the wave to slow down. This can cause re-entrant waves that spiral back around the tissue, causing the heart to beat much too quickly, which can be fatal,” said Dr. Gil Bub, lead author from Oxford University. “If we can control these spirals, we could prevent that,” he explained, noting the potential of optogenetics for controlling these abnormal waves.
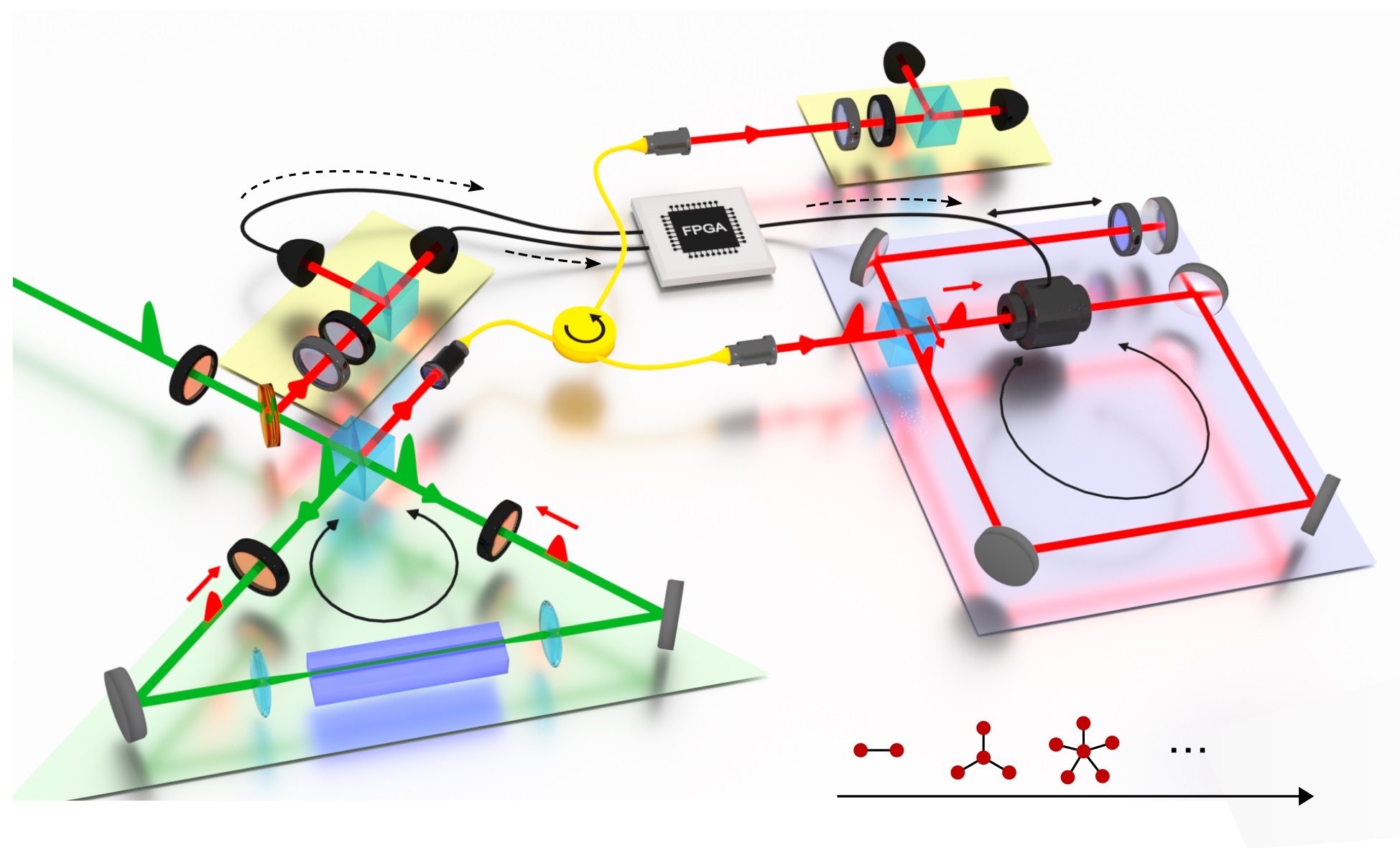
In their study, the researchers used a protein called channelrhodopsin, which was delivered to heart cells using gene therapy techniques to make them light-responsive. Then, using a computer-controlled light projector, the team was able to control the speed of the cardiac waves, their direction and even the orientation of spirals in real time – something that has never been shown before in a living system.
The ability to provide fine control means that researchers are able to carry out experiments at a level of detail previously only available using computer models. The finding also provides an experimental platform in which researchers can compare those models to experiments with real cells, potentially improving the understanding of how the heart works. The method can also be applied to the physics of such waves in other processes. The long-term goal would be to use optogenetics to develop precise treatments for heart conditions.
“The level of precision is reminiscent of what one can do in a computer model, except here it was done in real heart cells, in real time,” said Dr. Entcheva.
“Precise control of the direction, speed and shape of such excitation waves would mean unprecedented direct control of organ-level function, in the heart or brain, without having to focus on manipulating each cell individually,” she explained. “This ideal therapy has remained in the realm of science fiction until now.”
Dr. Entcheva and colleagues emphasize that there are significant hurdles before optogenetics can be used to offer new treatments. One key issue is being able to alter the heart to be light-sensitised and being able to get the light to desired locations. However, as gene therapy moves into the clinic and with miniaturization of optical devices, use of this all-optical technology may become possible. In the meantime, the research enables scientists to look into the physics behind many biological processes, including those in our brains and hearts.